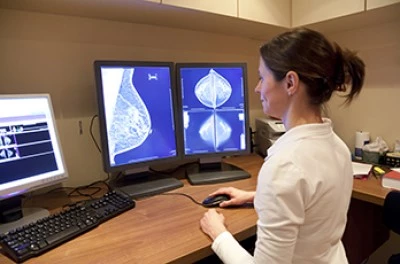
Diagnosing Breast Cancer

Breast cancer can be found by a symptom. Perhaps a lump, thickening of the skin, rash, or inflamed skin. It can also be detected by a test, such as a mammogram, ultrasound, or MRI. Even before an official breast cancer diagnosis, most young adults find it themselves. Signs and symptoms of breast cancer can include:
- a lump
- thickening of the skin
- rash
- dimpling of skin (like an orange peel)
- redness and swelling
- inverted nipple and itchy or scaly nipple
Get to know what is normal for you and see a doctor if you notice anything out of the ordinary. Current mammography guidelines recommend screening mammography starting at age 45 or 50, unless you are at high risk of the disease. So it's important to understand the breast cancer risk factors.
If you find something of concern, a mammogram, ultrasound or possibly MRI of the breast may be ordered. A mammogram is a low-dose x-ray of the breast used to look for presence of disease. In contrast, an ultrasound or sonogram uses high-frequency sound waves to create a picture of some part of the inside of the body. An MRI (Magnetic Resonance Imaging) uses magnetic field and radio waves to create a detailed picture of the organs and tissues in your body.
These tests or physical symptoms may indicate something suspicious, but only a biopsy (removal of all or part of the tumor for examination under a microscope) can tell you whether the problem is definitely breast cancer.
Common Tests After Breast Cancer Diagnosis
Once you have received a breast cancer diagnosis, you will likely undergo additional testing. This may include an MRI, mammogram or ultrasound of the other breast. Sentinel lymph node biopsy is also common. This relatively new technique allows a surgeon to “sample” your lymph nodes and determine whether breast cancer may have traveled there. In the procedure, blue dye is injected into the breast. After giving it time to travel to the lymph nodes, the surgeon removes only the lymph nodes in which the blue dye is found. These nodes will be sent to a pathologist for testing to see if cancer is present.
In addition, CT or CAT scans, PET scans and/or bone scans may be ordered to see if the cancer has spread to another part of the body. The most typical scans are:
Bone Scans
These scans reveal if cancer has spread to the bones. They look at the bones for “hot spots” that may reveal cancer. To conduct a bone scan, your healthcare provider injects dye, then waits a few hours for it to move through the bloodstream so it can be visible in the scan.
Chest X-Ray
A chest x-ray may reveal if breast cancer has spread to the lungs.
CT/CAT Scan (Computerized Tomography or Computerized Axial Tomography)
This scan provides a more-detailed x-ray of the body, usually in order to see if cancer has spread to the brain, lungs and/or liver. Before the scan, you will either ingest a contrast dye and/or have it injected into a vein. The dye highlights specific areas of the body more clearly. A computer rotates around the body, creating a three-dimensional image.
Liver Scan
A liver scan involves having a contrast dye injected into the vein. The dye will collect in areas where there is activity that could indicate cancer growth.
MRI (Magnetic Resonance Imaging)
Before an MRI, you will receive an injection of a contrast dye, then lie down inside a tube-like machine that uses radio waves and a powerful magnet linked to a computer to take three-dimensional pictures of your body.
PET Scan (Positron-Emission Tomography)
This scan works by monitoring the use of glucose (a source of energy) throughout the body. Cancer cells use more glucose than normal cells do. Before the scan, you will have some radioactive glucose called a “tracer” injected into a vein. A computer then takes images and looks for the areas using the most glucose. The PET scan can sometimes find cancer that other tests miss.
PET CT Scan
A combination of the PET and CT Scans, performed at the same time, can present a more detailed image of the presence or extent of cancer in the body.
Genetic testing may be offered or ordered to determine if your cancer is due to an inherited genetic mutation.
Finally, before starting chemotherapy, a test to determine your risk of recurrence may be ordered. The most common tests, Oncotype, Mammaprint and Mammastrat, involve examining a piece of the patient’s tumor to estimate the risk of recurrence if no additional treatment (beyond surgery) is received. These tests provide guidance on whether chemotherapy should be recommended.
Coping with “Scanxiety”
We know that any type of testing can make you anxious and stressed. This is normal. Know that these tests help to determine whether you have the disease and, if so, the best breast cancer treatment plan for your particular situation. We can offer support to help you cope with testing anxiety:
- Online Support: Chat online with other young women who have experienced testing anxiety.
- Peer Mentors: Talk one-on-one over the phone to another woman who has been there.
- Face 2 Face Networks : Meet up with young survivors in your community.
Newly Diagnosed Navigator
Learn to navigate your breast cancer diagnosis and treatment in an easy-to-understand format that includes inspiring messages from young adults who’ve been down this road.